
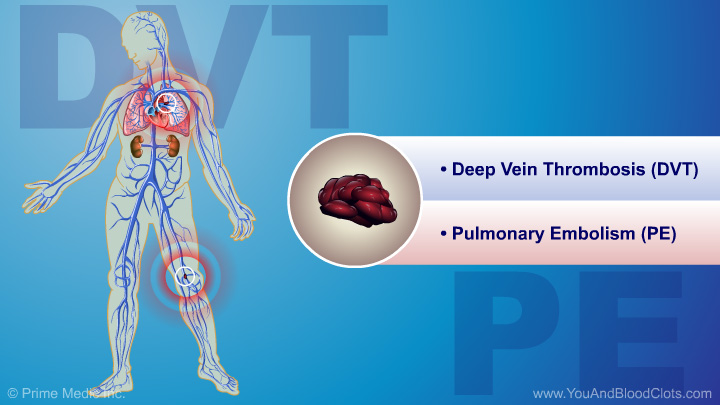



Watch this slide show to learn about the risk factors, causes, symptoms, and diagnosis of dangerous VTE blood clots. Venous thromboembolism (VTE) is a term that includes both deep vein thrombosis and pulmonary embolism. When a blood clot forms in a deep vein in the body, it is called deep vein thrombosis (DVT). When that blood clot breaks off and travels to the lungs it is called a pulmonary embolism (PE).
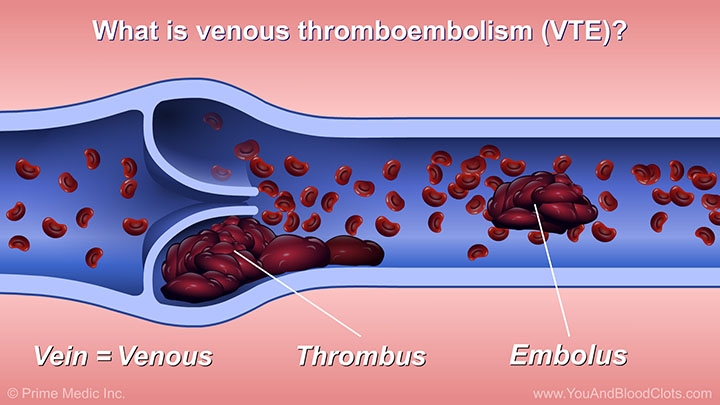
Venous thromboembolism (VTE) is a term that includes both deep vein thrombosis and pulmonary embolism. When a blood clot forms in a deep vein in the body, it is called deep vein thrombosis (DVT). When that blood clot breaks off and travels to the lungs it is called a pulmonary embolism (PE). Watch this animation to learn about the risk factors, causes, symptoms, and diagnosis of dangerous VTE blood clots.
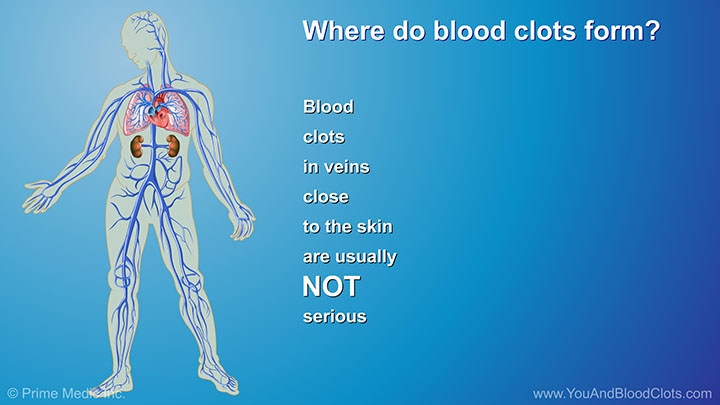
When a blood clot forms in the veins of the body it’s called VTE, or venous thromboembolism. In this video, expert pulmonologist Dr Sandra Adams explains what VTE is and also describes the three types of VTE: (1) superficial vein thrombosis, (2) deep vein thrombosis (DVT) and (3) pulmonary embolism (PE). DVT and PE are the most dangerous types of VTE.
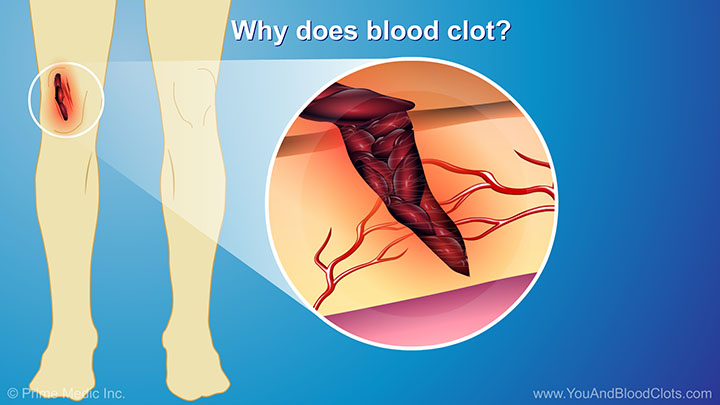
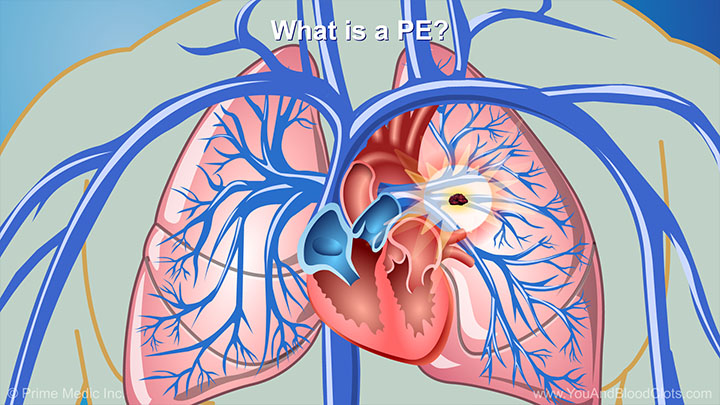
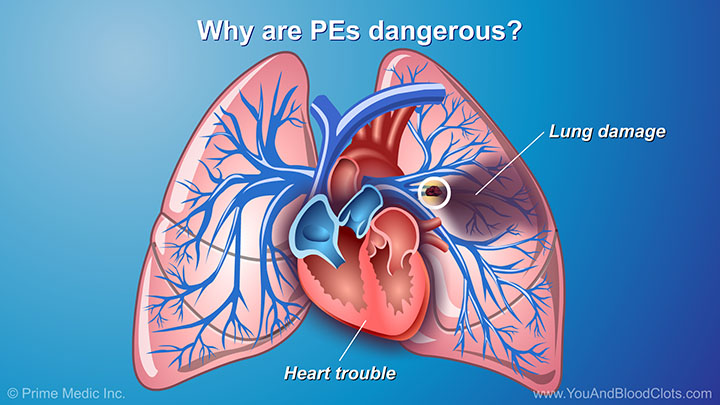
In this video, Dr Sandra Adams explains what blood clots are and when they can be dangerous. When we get injured, blood clots normally form in the body to help stop bleeding. They usually go away once the body has healed. Dr Adams explains that blood clots that form in the deep veins can block blood flow, and might cause pain or swelling. A blood clot can be very dangerous if it breaks off from one of the deep veins and moves through the bloodstream into the vessels of the lungs. This clot blocks blood from moving normally through the vessels of the lungs and can cause low oxygen and even death.
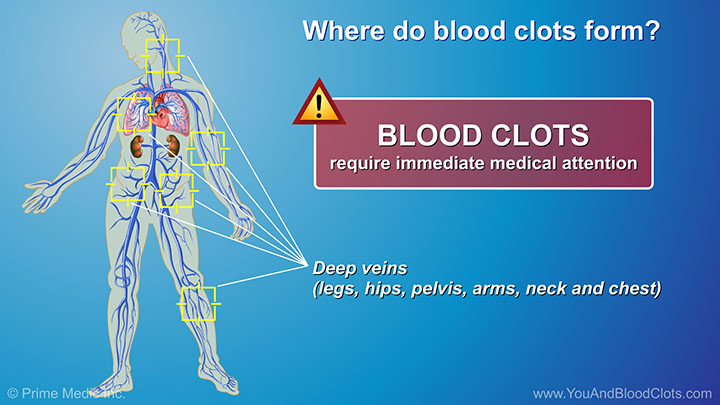
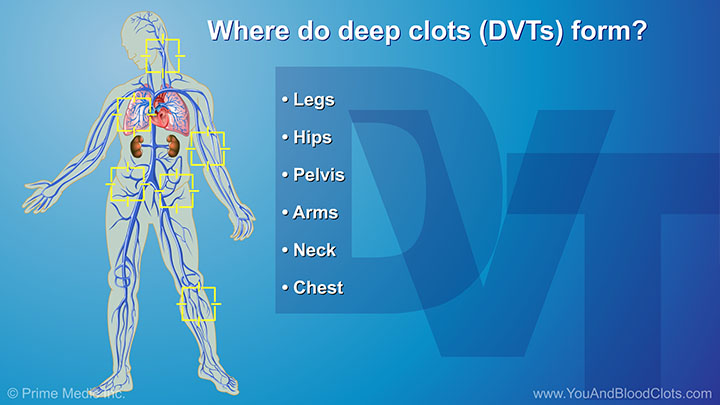
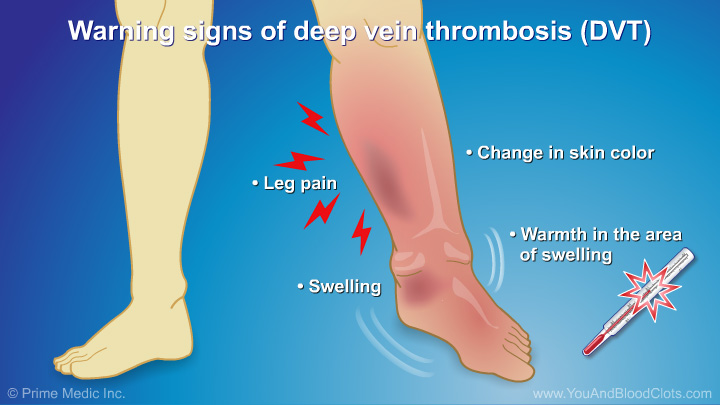
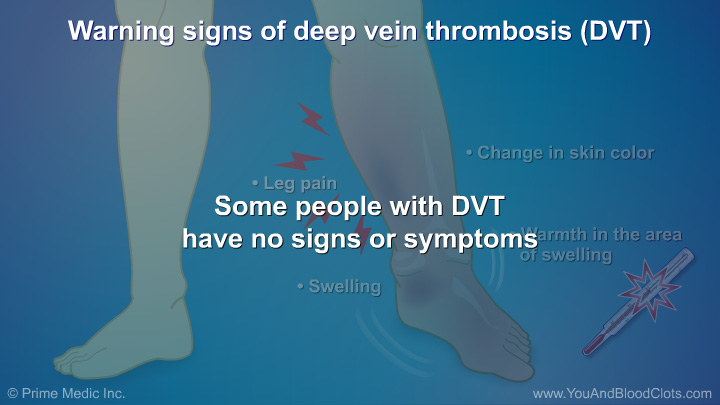
Deep vein thrombosis (DVT) is a blood clot that forms in a vein deep in the body. In this video, Dr Sandra Adams explains that these kinds of clots most often form in the legs, hips or pelvis but sometimes in the arms, neck or chest area. These deep clots can clog up the veins and slow down the blood flow. Common symptoms or warning signs of DVT are swelling in one leg, pain in one leg, and/or a change in color such as redness of the skin close to the blood clot. Sometimes the skin around the swollen area feels warm to touch. If you have any of these problems, you should get medical help as soon as possible.
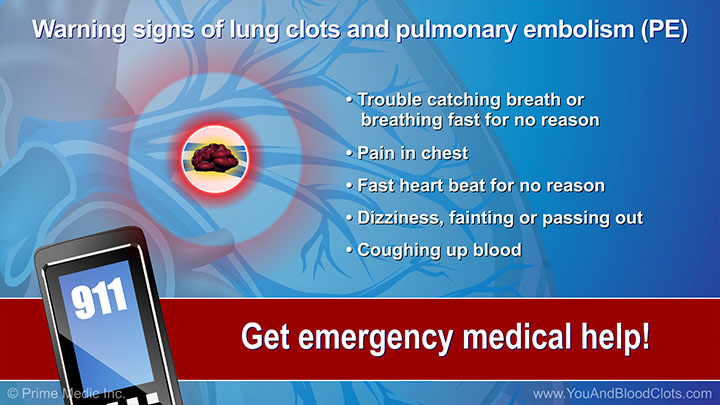
When a blood clot travels through the bloodstream to the vessels of the lungs it is called a pulmonary embolism (PE) and it can cause a lot of problems, as pulmonologist Dr Sandra Adams explains in this video. The most common signs and symptoms include shortness of breath, cough, chest pain (particularly when breathing in), coughing up blood, fainting or feeling dizzy, breathing fast or having a fast heartbeat for no reason. A PE is an emergency and requires immediate medical attention. The good news is that if a PE is recognized quickly and you get the right care, you can recover from it. If you have any signs of a dangerous blood clot, see your doctor or call 911 immediately.
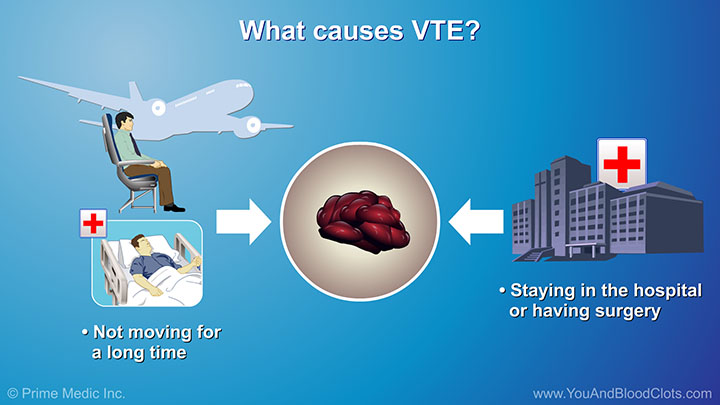
In this video, Dr Sandra Adams describes who is at risk for VTE blood clots. While dangerous blood clots can happen to anyone, three kinds of risk factors make them more likely to occur. The first is not moving for a long time. This may happen when someone cannot move because of injury, illness or hospitalization. Lack of movement could also come from simply sitting too long when working, watching TV, or traveling by car or plane. The second risk factor for VTE is having too many things in the blood, called clotting factors that cause the blood to clot more than usual. Examples of this include: taking birth control pills, smoking, having cancer, inheriting a condition from your parents or getting a disease that causes an imbalance of these clotting factors in the body. The third risk factor for VTE blood clots is damage to blood vessels. Physical injury to a blood vessel, such as damage or scarring caused by an intravenous, or IV catheter, a broken bone, or a previous blood clot can make VTE blood clots more likely. The more of these factors someone has, the higher the risk of developing dangerous blood clots or VTE.
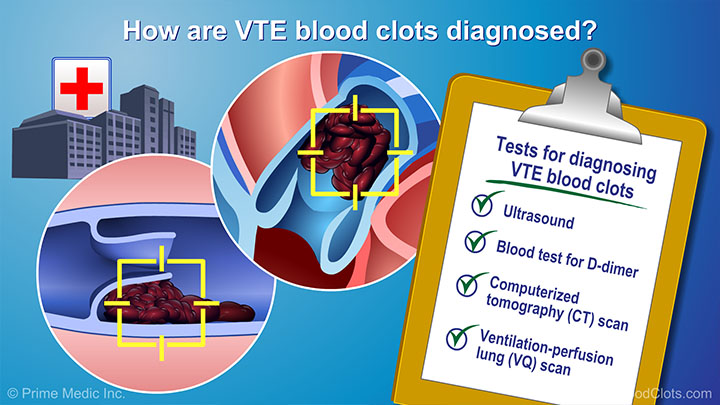
In this video, expert physician Dr Sandra Adams describes the common tests and procedures that are used to diagnose venous thromboembolism (VTE). If you have signs of a DVT blood clot in the leg, hip or pelvis, or in the arm, neck or chest, your doctor may order an ultrasound of the deep veins. If you have signs of a pulmonary embolism, or PE, your doctor may order a CT scan of the chest with IV contrast or a VQ scan of the chest. Also, an ultrasound of the heart (called an echocardiogram or echo for short) can sometimes discover a blood clot in the lungs.
As Dr Sandra Adams explains in this video, it is important to recognize a DVT and PE blood clot right away so that it can be treated as soon as possible and so that damage can be kept to a minimum. Prompt diagnosis and treatment can prevent scarring of the blood vessels and may keep additional clots from forming. Without treatment, blood clots can cause life-long health problems and can be life threatening. Recognizing and getting treatment for a dangerous clot early is your best defense.
VTE, DVT and PE can be difficult to diagnose and a number of other conditions can cause the same or similar symptoms, explains Dr Sandra Adams in this video. While some patients may have several symptoms of VTE, others may only have a few symptoms, or may not be aware of what is happening to them. If you think you may have a dangerous blood clot, seek medical help right away. Write down your symptoms so you can discuss them with your doctor. If you know you have risk factors for VTE blood clots (such as having recently been in the hospital, suffered an injury, taken a long trip, or if you have previously had a dangerous blood clot) be sure to tell your healthcare provider.
In this video, Dr Sandra Adams describes how family members, caregivers and friends can support people with VTE blood clots by being aware of the symptoms, risk factors, and understanding the importance of receiving the right treatment quickly. For patients who have had surgery, family members or caregivers can help by reminding patients to be as active as possible and take any medicines or therapy, recommended by their physician.
Jointly provided by Postgraduate Institute for Medicine, WipeDiseases Foundation and Prime Medic Inc.
This activity is supported by an independent educational grant from Daiichi Sankyo.
This website is part of the Animated Patient™ series developed by Prime Medic Inc., to provide highly visual formats of learning for patients to improve their understanding, make informed decisions, and partner with their healthcare professionals for optimal outcomes.